How molecular glues protect insulin-producing cells from diabetic damage
The researchers have discovered a novel approach to protecting insulin-producing beta cells from the damaging effects of glucolipotoxicity—a harmful condition linked to the progression of type 2 diabetes (T2D). These findings, published in Nature Communications, could lead to promising treatments targeting beta cell dysfunction.
For patients, this research could lead to new treatments that protect the insulin-producing cells in the pancreas, potentially slowing or even preventing the progression of diabetes, thus reducing the need for insulin therapy and improving long-term blood sugar control. Unlike current therapies that primarily manage blood sugar levels, this approach would allow doctors to directly target beta cell loss, which could improve long-term disease outcomes for their patients.
“This is an exciting step forward in our understanding of beta cell protection and the prevention of diabetes deterioration,” said the lead author. “For the first time, we’ve shown that it’s possible to use small molecules to fine-tune carbohydrate response element binding protein (ChREBP) activity in a way that could have major therapeutic implications.”
More than 500 million people worldwide are living with diabetes, a disease characterized by high blood sugar levels due to insulin resistance and/or beta cell failure. In T2D, long-term exposure to high glucose and fatty acid levels (glucolipotoxicity) can ultimately lead to beta cell dysfunction and death.
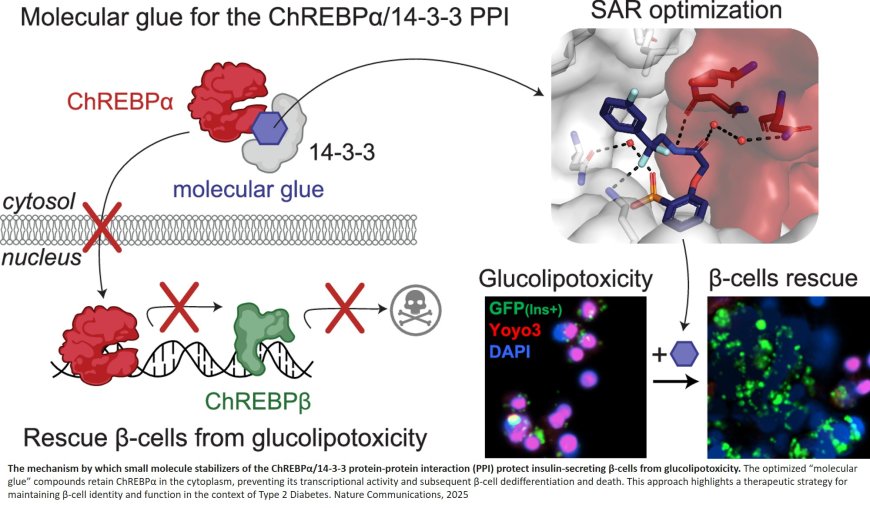
ChREBP is a transcription factor that plays a crucial role in regulating glucose metabolism. It exists in two main isoforms: ChREBPα and ChREBPβ. This is the first study to identify and develop small molecules—termed "molecular glues"—that enhance the interaction between ChREBPα and 14-3-3 proteins in pancreatic beta cells.
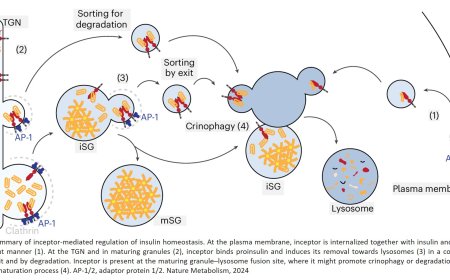
The molecular glues in this case increase the binding between 14-3-3 proteins and ChREBPα, which is anchored in the cytoplasm of the beta cell by the 14-3-3 proteins. Under conditions of glucolipotoxicity, ChREBPα goes into the nucleus and starts making too much of ChREBPβ, which acts to disable and even kill the patient’s beta cells. By using a molecular glue designed to increase the binding of ChREBPα to 14-3-3 proteins, ChREBPα never leaves the cytoplasm, cannot enter the nucleus, and therefore does not make ChREBPβ.
When tested in primary human beta cells, these molecular glues significantly reduced the toxic effects of glucolipotoxicity, thus preserving beta cell function and identity. This discovery represents a major shift in diabetes research, as transcription factors like ChREBP have long been considered "undruggable" targets. The study also highlights the broader potential of molecular glues for modulating similar interactions in other diseases.
“Our findings suggest a completely new strategy for preserving beta cell function in diabetes,” said the senior author. “This approach could complement existing diabetes treatments and help prevent disease progression.”
Researchers are now working to refine these compounds and evaluate their potential for clinical translation. Future studies will focus on optimizing the molecular glues for therapeutic use and testing them in preclinical diabetes models.
https://www.nature.com/articles/s41467-025-57241-7
https://sciencemission.com/protect-beta-cells-from-glucolipotoxicity