Anticancer antibodies can cause autoimmune brain disease
Consider two seemingly unrelated medical puzzles. First: Every day, our bodies produce hundreds of billions of new cells, many of which are mutated. If cancer arises from cellular mutation, why don’t we all have the disease all the time? Second: Severe autoimmune conditions like lupus and multiple sclerosis often strike without warning. No one knows what triggers them.
A new study published in Nature, suggests the two puzzles may be directly connected. The research reveals that our immune system is pre-equipped with antibodies that can both fight tumors and attack the brain.
“Patients with autoimmune diseases often experience the condition coming out of nowhere,” says the lead author of the study. “It may be from the cancer you never knew you had.”
The team focused on anti-NMDA receptor encephalitis (ANRE), the debilitating autoimmune brain disease. In ANRE, the immune system attacks proteins in the brain called NMDA receptors, causing psychosis, insomnia, and seizures. Many patients with this condition are found to have a tumor that produces the same NMDA receptors, but outside the brain.
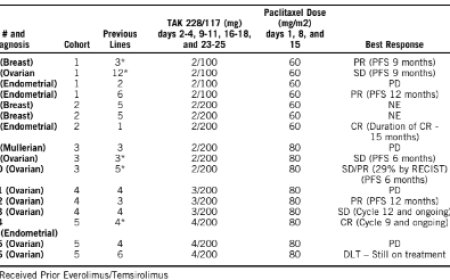
Using a mouse model of breast cancer, the team traced antibodies from precursors present at birth through their evolution within the tumor into potent cancer-killing molecules. The mice that developed the strongest antibody responses saw their tumors shrink spontaneously. However, when those same antibodies were infused into the brains of healthy mice, they caused seizures and elevated body temperatures, mirroring what patients with ANRE experience.
Using a method called cryo-EM, the authors realized that some antibodies activated NMDA receptors and others inhibited them. “This means that the same immune response against a tumor can produce antibodies with completely opposite effects on the brain,” The author explains. “Understanding which antibodies are harmful and which are protective could eventually help us develop treatments that preserve the immune system’s cancer-fighting abilities while preventing neurological damage.”
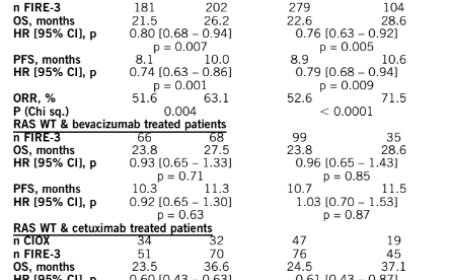
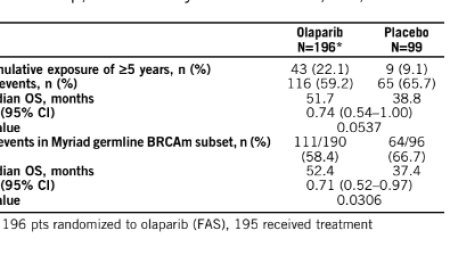
With this goal in mind, the team turned their attention to the clinic. The researchers found that NMDA receptor proteins are commonly produced by tumors in patients with triple-negative breast cancer, a disease known to resist hormone therapy and other common forms of treatment. About 15% of these patients had formed antibodies targeting NMDA receptors. Notably, these patients tended to have better clinical outcomes, suggesting that their immune systems were actively fighting the cancer.
“With this knowledge, we can now begin carefully designing antibody-based drugs that could one day be used to treat patients with triple-negative breast cancer,” says the senior author. “Our research shows that while cancer remains deeply puzzling, considering the whole-body response to the disease may help us solve biomedical mysteries that have eluded scientists for decades.”