Gestational diabetes therapeutics

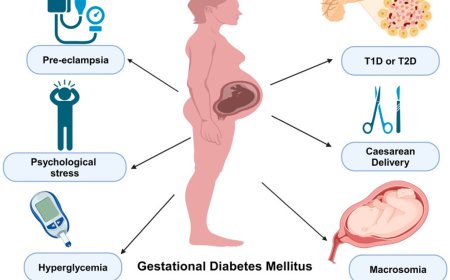
Gestational diabetes mellitus (GDM) is a condition characterized by high blood sugar levels that are first recognized during pregnancy. Here are some current and emerging therapeutics for GDM:
Lifestyle Interventions
1. Dietary modifications: Healthy eating habits, such as reducing sugar and refined carbohydrate intake, can help manage blood sugar levels.
2. Physical activity: Regular physical activity, such as walking and swimming, can improve insulin sensitivity.
3. Weight management: Maintaining a healthy weight can reduce the risk of developing GDM.
Pharmacological Therapies
1. Insulin therapy: Insulin is the primary treatment for GDM, especially for women with high blood sugar levels or those who cannot manage their condition through lifestyle modifications alone.
2. Metformin: Metformin is an oral anti-diabetic medication that can be used to treat GDM, especially for women with mild GDM.
3. Glyburide: Glyburide is an oral anti-diabetic medication that can be used to treat GDM, especially for women with mild GDM.
Emerging Therapies
1. Incretin-based therapies: Incretin-based therapies, such as GLP-1 receptor agonists, may be effective in managing GDM.
2. SGLT2 inhibitors: SGLT2 inhibitors, which reduce glucose reabsorption in the kidney, may be effective in managing GDM.
3. Probiotics: Probiotics may have a beneficial effect on glucose metabolism and insulin sensitivity in women with GDM.
Alternative Therapies
1. Acupuncture: Acupuncture may have a beneficial effect on glucose metabolism and insulin sensitivity in women with GDM.
2. Yoga: Yoga may have a beneficial effect on glucose metabolism and insulin sensitivity in women with GDM.
3. Mindfulness-based interventions: Mindfulness-based interventions may have a beneficial effect on glucose metabolism and insulin sensitivity in women with GDM.
Future Directions
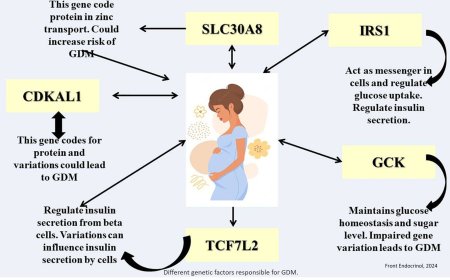
1. Personalized medicine: Tailoring therapies to individual patients based on their genetic and phenotypic profiles.
2. Biomarkers: Identifying biomarkers to predict GDM and monitor disease progression.
3. Epigenetic therapies: Targeting epigenetic changes to improve insulin sensitivity and reduce inflammation.
Current Guidelines
1. American College of Obstetricians and Gynecologists (ACOG): Recommends screening for GDM at 24-28 weeks of gestation.
2. American Diabetes Association (ADA): Recommends screening for GDM at the first prenatal visit, with repeat screening at 24-28 weeks of gestation if necessary.
Key Considerations
1. Fetal monitoring: Regular fetal monitoring is essential to ensure the health and well-being of the fetus.
2. Postpartum care: Women with GDM require postpartum care to monitor for the development of type 2 diabetes.
3. Lactation support: Women with GDM should receive lactation support to promote breastfeeding, which can help reduce the risk of developing type 2 diabetes.