Hyperinnervation causes scar at the wounded skin
A new study published in Cell reveals a way to fully regenerate skin by unblocking an embryonic healing mechanism that shuts off after birth. Demonstrated on mice, the study suggests a potential means to develop similar therapies in human patients.
“Essentially, we found a way to make wound healing outcome a lot better by learning how embryos do this so well,” said the senior author of the new study. “I'm excited because we pushed the needle in a really important direction. When we have a wound, most skin cell types cannot regenerate and we get a scar. But now I think we've found a way to change that, so that many cell types can regenerate and we don't get a scar.”
Skin is often touted as the prime example of an organ that can regenerate itself. In truth, the healing is not entirely skin deep.
After injury, epidermal stem cells reseal the surface and fibroblasts deposit dense collagen scar tissue. But skin also contains an array of other cells (somewhere between 10 and 50 types, depending on how they are classified) including hair follicles, vascular and lymphatic vessels, sweat glands, pigment cells, immune cells, fat cells, and nerves. Most of these other types fail to regenerate so the scarred skin remains fundamentally altered.
Earlier studies had shown that embryonic wounds could heal without scarring, but the new study reveals far more. After injury, embryonic skin restores all cell types but this ability fades quickly after birth. The study reveals the molecular mechanisms behind this switch—and how to turn them back on.
“Our findings suggest that some organs retain an inherent regenerative potential that is simply held in check — and that removing this block may be sufficient to allow regeneration to occur,” the author said. “In other words, regeneration may not need to be built anew, but simply set free.”
To investigate wound healing, the team used a biopsy punch tool to remove a full thickness piece of skin and then compared how the organ regenerated in embryonic mice and postnatal mice at several timepoints.
One challenge was keeping track of the locations of the embryonic wounds because they healed so completely that they became indistinguishable from normal skin. The scientists marked the injury sites with fluorescent beads and henna ink.
They found that the ability to regenerate skin steadily decreased in the days after birth. The most dramatic shift occurred from three days before birth to five days afterwards—a window of only eight days.
In mice wounded three days before birth, the skin regenerated diverse cell types and closely resembled unwounded skin. But when wounded at five days after birth, the site was covered by epithelial cells and became packed with collagen scar tissue and abnormally dense nerve fibers and immune cells; many other skin cell types failed to regrow.
Next the team sought to identify the key drivers behind these differences in regeneration.
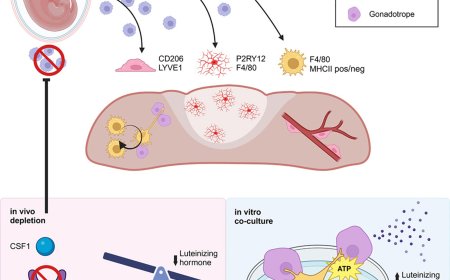
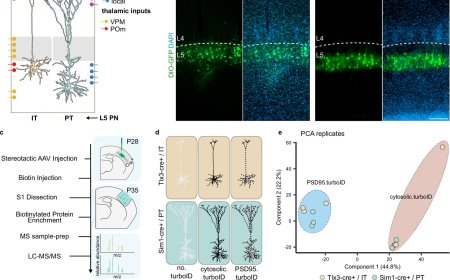
They found that postnatal wound sites became densely packed with nerves. This “hyperinnervation” occurs because fibroblasts in postnatal wounds upregulate the gene Cxcl12, which recruits excessive nerves to the injury site and impairs the regrowth of other skin cell types.
When researchers depleted Cxcl12 in wounds in postnatal mice, the “hyperinnervation” was curtailed and the skin regrew diverse cell types. Blocking local nerve signaling with botulinum toxin A (Botox) produced similar effects.
“The surprising part is that we identify a block” said the author. “And this block is through fibroblast-nerve interaction. The relationship between those two different cell types has not been the focus in wound healing studies. I feel that this is very helpful to the field, because now we can really consider these two as actual communicators."
https://www.cell.com/cell/fulltext/S0092-8674(26)00234-5
https://sciencemission.com/Hyperinnervation-inhibits-organ-level-regeneration